We're loading the full news article for you. This includes the article content, images, author information, and related articles.
From painkillers to antibiotics, doctors warn that self-medication delays treatment and worsens outcomes.
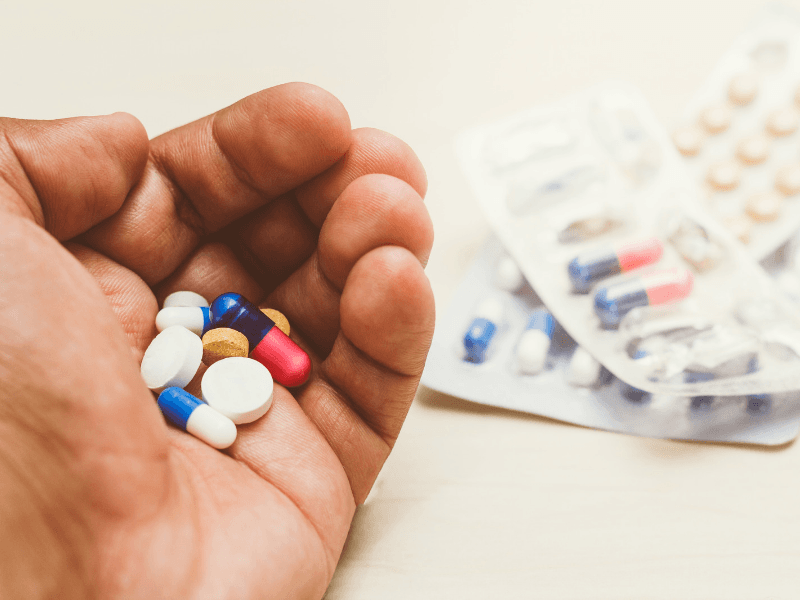
Kenya. A headache appears, so you buy painkillers. A cough begins, so you pick up “something strong.” A fever rises, so you take antibiotics—often without a prescription—hoping to stop the illness quickly. This routine has become normal across many communities because it feels fast, affordable, and convenient. But doctors warn that self-medication is quietly driving late hospital visits in Kenya, turning manageable illnesses into complicated emergencies and worsening outcomes for patients and families.
At HAMAT Hospital, clinicians describe a common story: a patient arrives after days or weeks of self-treatment, when symptoms have progressed into severe dehydration, persistent infection, uncontrolled blood pressure, or complications affecting breathing, kidneys, or the nervous system. In many cases, what made the situation dangerous was not the first painkiller. It was the delay—masking symptoms while the disease continued.
Medical experts explain that symptoms are the body’s signals. Pain, fever, fatigue, dizziness, and cough are not random inconveniences; they are information. Self-medication often reduces discomfort temporarily, which can create false reassurance. The illness then advances quietly, and the person seeks care only when the body can no longer compensate.
Doctors warn that this pattern is particularly risky when antibiotics are used incorrectly. Antibiotics do not treat viral infections such as the common cold, yet many people take them for flu-like illnesses. Misuse can also occur when the wrong antibiotic is chosen, the dose is inconsistent, or the course is stopped early because symptoms improved. The result is not only individual harm; it also fuels the broader threat of antimicrobial resistance, where bacteria become harder to treat.
1) The misdiagnosis trap. Fever is often assumed to be malaria; stomach pain is assumed to be ulcers; dizziness is assumed to be “low pressure.” But the same symptom can have multiple causes. Treating the wrong cause wastes time and can allow disease to progress. A cough treated repeatedly with antibiotics might actually be allergy, asthma, or viral infection. Recurrent headaches treated as stress might be driven by blood pressure, anemia, or vision problems.
2) The delay trap. Many patients seek care only after symptoms become unbearable. Doctors emphasize that early care is often simpler and cheaper. When the delay extends, the condition may require more testing, stronger treatment, or admission. The cost is not only financial—it is also time away from work, school, and caregiving.
3) The side-effect trap. Over-the-counter medicines are useful when used appropriately, but repeated or unsupervised use can cause harm. Some painkillers can irritate the stomach lining and increase ulcer risk. Others can strain the kidneys, especially when a person is dehydrated. Mixing multiple cold-and-flu products can accidentally duplicate ingredients and increase risk. Doctors see patients who arrive with complications that began as “just managing symptoms at home.”
One of the most dangerous illusions of self-medication is short-term improvement. A fever may reduce after medication, but the underlying infection may still be present. Pain may subside, but the condition causing pain may still be worsening. Clinicians emphasize that recurring symptoms—especially those that return quickly—often mean the root cause was not addressed.
Another blind spot is the assumption that pharmacies can replace clinical assessment. Pharmacists play an important role in safe medicine use, but diagnosis requires history, examination, vital signs, and sometimes testing. When symptoms are persistent, progressive, severe, or unusual, the safer next step is a walk-in consultation.
Doctors advise walking in for assessment when:
In a properly equipped hospital, clinicians start with triage: checking vital signs and identifying risk early. A focused consultation follows—what started when, what has changed, what has been taken, and what symptoms are accompanying the main complaint. When needed, targeted tests are used to confirm diagnosis rather than guess. This protects patients from unnecessary drugs, reduces the risk of missed serious conditions, and supports better outcomes.
Doctors stress that timely care is not about overreacting. It is about preventing small problems from becoming life-altering crises. In many cases, a walk-in visit provides reassurance, correct diagnosis, and a clear plan—something no self-medication routine can reliably replace.
When to walk in: Persistent symptoms, worsening pain, unexplained fatigue or fever should be medically reviewed rather than managed at home.
Medical professionals advise visiting a properly equipped hospital for assessment, testing and follow-up care.
Keep the conversation in one place—threads here stay linked to the story and in the forums.
Sign in to start a discussion
Start a conversation about this story and keep it linked here.
Other hot threads
E-sports and Gaming Community in Kenya
Active 9 months ago
The Role of Technology in Modern Agriculture (AgriTech)
Active 9 months ago
Popular Recreational Activities Across Counties
Active 9 months ago
Investing in Youth Sports Development Programs
Active 9 months ago