We're loading the full news article for you. This includes the article content, images, author information, and related articles.
A critical analysis of Kenya's health crisis reveals a deadly combination of preventable maternal issues and a rising toll of non-communicable diseases.
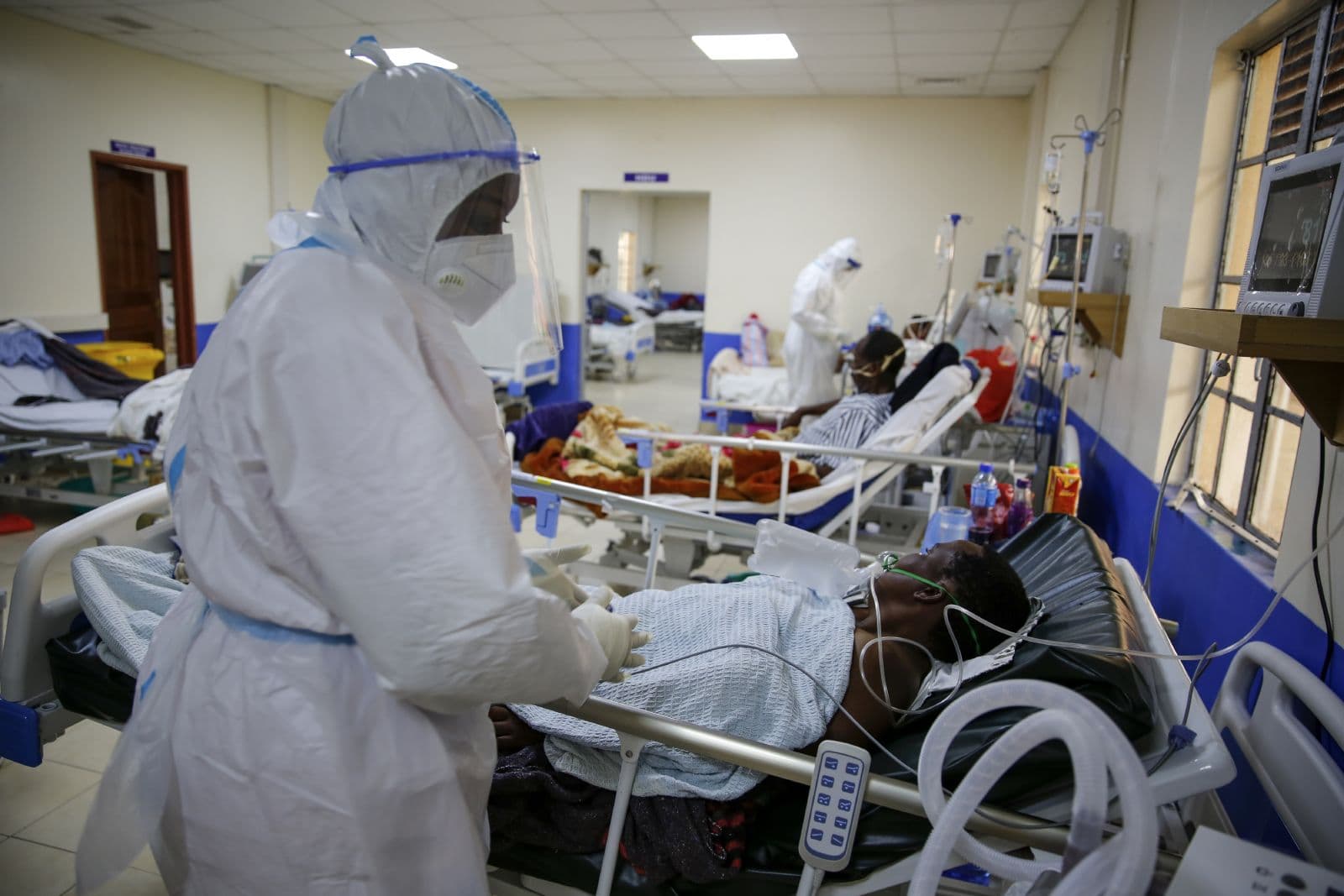
A critical analysis of Kenya's health crisis reveals a deadly combination of preventable maternal issues and a rising toll of non-communicable diseases.
Kenya stands at a critical juncture in its public health trajectory. Despite impressive gains in overall life expectancy, the nation is battling a dual-front medical crisis.
A deep dive into national health data reveals a harrowing reality: Kenyans are dying concurrently from easily preventable traditional complications and a devastating surge in modern, non-communicable diseases (NCDs). The healthcare infrastructure is buckling under this immense pressure.
The epidemiological shift in Kenya is stark and alarming. Non-communicable diseases—primarily cardiovascular conditions, diabetes, cancer, and severe mental health disorders—now account for nearly 40 percent of all mortalities across the nation. This surge is intrinsically linked to rapid urbanization, shifting dietary habits, and increasingly sedentary lifestyles. The burden is no longer confined to the affluent urban elite; it has deeply penetrated rural populations who lack access to the specialized care required for these chronic conditions.
The cost of treating NCDs is catastrophic for the average Kenyan family. Cancer treatments and lifelong diabetes management routinely push households into severe poverty. The national healthcare system, historically oriented towards combating infectious diseases like malaria and HIV/AIDS, is ill-equipped to handle the specialized diagnostic and long-term care demands of the NCD epidemic. Essential medications are frequently out of stock, and specialist oncologists and cardiologists remain concentrated in the capital.
Tragically, as the nation grapples with these new threats, it continues to lose lives to entirely preventable causes. Maternal mortality remains unacceptably high. Women are dying from excessive bleeding after delivery, pre-eclampsia, and obstructed labour. These are not mysterious or incurable conditions; they are emergencies that basic, well-resourced medical facilities can effectively manage.
The persistence of these deaths points directly to systemic failures: inadequate rural clinics, lack of emergency transport, and a critical shortage of trained midwives and doctors. The National Council for Population and Development explicitly notes that these deaths are not inevitable; they are the direct result of resource misallocation and a lack of sustained political will to fortify primary healthcare at the grassroots level.
The health crisis is exacerbated by a population growing faster than the expansion of medical services. Addressing this requires a radical departure from current public health strategies. It demands aggressive investment in preventive healthcare, comprehensive public education on lifestyle diseases, and the equitable distribution of medical personnel and equipment.
Leaders must be held accountable for bridging the glaring inequalities that dictate who lives and who dies in Kenya. A robust healthcare system is not a luxury, but a fundamental pillar of national economic stability and human dignity.
"The data shows us that the deaths we are seeing today are not inevitable; they are a tragic reflection of preventable systemic failures."
Keep the conversation in one place—threads here stay linked to the story and in the forums.
Sign in to start a discussion
Start a conversation about this story and keep it linked here.
Other hot threads
E-sports and Gaming Community in Kenya
Active 9 months ago
The Role of Technology in Modern Agriculture (AgriTech)
Active 9 months ago
Popular Recreational Activities Across Counties
Active 9 months ago
Investing in Youth Sports Development Programs
Active 9 months ago