We're loading the full news article for you. This includes the article content, images, author information, and related articles.
A woman from Worcestershire who has lived with a \"debilitating\" and \"agonising\" condition for 23 years has set herself the challenge of raising money for the team that helped diagnose her. Harriet Amos, a musician and teacher from Worcester, was diagnosed with endometriosis in 2016 and has since undergone five operatio
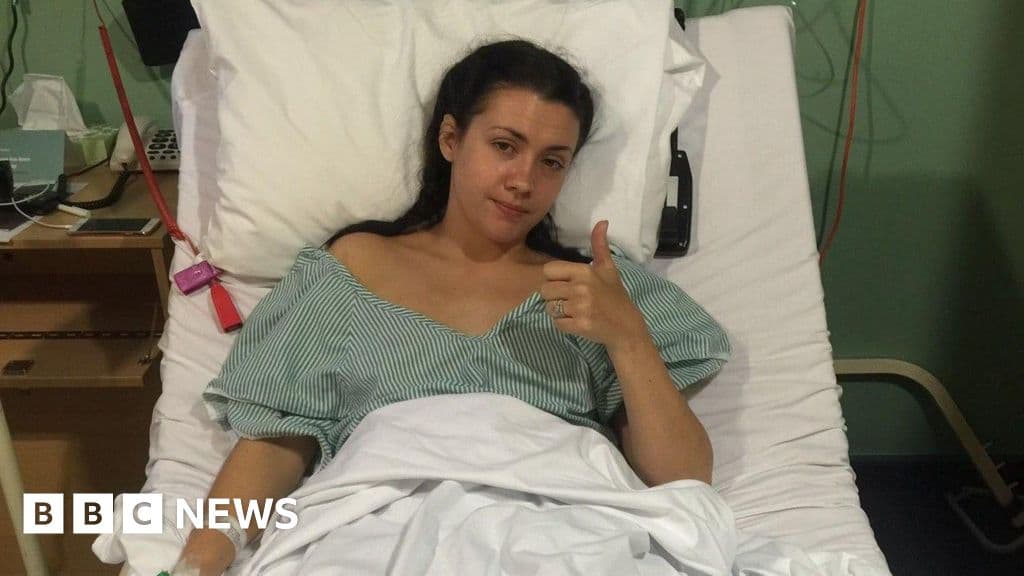
The silence surrounding chronic pelvic pain is being shattered by individual acts of resilience. Harriet Amos, a musician and educator in Worcestershire, has spent twenty-three years navigating a labyrinth of medical uncertainty, misdiagnosis, and surgical intervention. Today, her decision to leverage her professional network to fundraise for the hospital that eventually diagnosed her condition serves as a poignant indictment of a global healthcare system that frequently leaves women waiting years for critical answers.
For millions of women worldwide, the journey Amos has endured is not an anomaly but a standard, frustrating reality. Endometriosis, a systemic condition where tissue resembling the uterine lining grows outside the uterus, affects an estimated one in ten women globally. The stakes are immense: without early intervention, the disease leads to chronic, debilitating pain, significant mental health strain, and, in many cases, long-term fertility issues. The fundraising efforts led by Amos are not merely an act of gratitude they are a necessary intervention in a landscape where public health funding for reproductive care consistently lags behind demand.
The medical community has long struggled to quantify the true scale of the endometriosis crisis, largely because of the diagnostic delay. In the United Kingdom, patients can wait nearly a decade for an accurate diagnosis, a timeline that mirrors the experience of women across much of the developed world. This delay is attributed to a pervasive culture of normalizing menstrual pain, which often leads physicians to misattribute symptoms to gastrointestinal or psychological issues rather than exploring pelvic pathology.
Amos, who was eventually diagnosed in 2016, has undergone five separate surgical procedures, including the removal of an ovary. These interventions, while life-saving, highlight the aggressive nature of the disease when left to progress. The psychological toll of such a journey is equally severe, with patients reporting high rates of anxiety and depression directly correlated to the struggle for medical legitimacy. When a patient is forced to become their own advocate, the system has effectively failed to provide basic care.
The impact of endometriosis transcends the individual patient. It creates a significant drag on economic productivity, leading to high absenteeism and presenteeism in the workforce. In the UK, the annual economic burden of the condition is estimated to be in the billions of pounds. When converted to local currency, this represents a staggering economic drain, illustrating why reproductive health funding should be viewed as an investment in national productivity rather than an elective expense.
The disparity in care is even more pronounced in developing nations, including Kenya. While the United Kingdom possesses an established NHS infrastructure—however strained—women in East Africa often face a total absence of sub-specialized endometriosis care. Diagnostic laparoscopy, the gold standard for confirmation, remains inaccessible for the majority of the population outside of major urban hubs like Nairobi. The stigma surrounding menstrual health further complicates the issue, preventing many women from seeking even primary care until the condition has reached an advanced, agonizing stage.
The initiative led by the Worcestershire Acute Hospitals NHS Trust highlights a critical model for community-based healthcare improvement. By utilizing charitable funds to enhance patient comfort—such as the purchase of reclining chairs for patients suffering from acute pelvic pain—the trust is addressing the immediate, tangible needs of those in crisis. Joanna Street, a lead specialist nurse, notes that these small, donor-funded improvements dramatically alter the experience of patients arriving in emergency settings.
However, analysts argue that relying on charitable concerts and individual fundraising to bridge infrastructure gaps is a dangerous precedent. While admirable, the success of such initiatives should not obscure the need for structural government policy changes. As climate change and environmental toxins are increasingly investigated for their potential role in hormonal disruption, the incidence of endometriosis may rise, demanding a more robust public health response than charity alone can provide.
For Harriet Amos and thousands like her, the goal is not just to pay for a chair in a waiting room it is to ensure that the next generation does not have to endure the same multi-decade struggle for recognition. By increasing the profile of the condition, activists are forcing a shift in clinical education and public awareness. The path forward requires a unified approach: medical institutions must prioritize gynecological sub-specialties, governments must increase funding for reproductive health, and society must finally abandon the archaic notion that chronic pelvic pain is an inevitable component of womanhood. The journey toward equity in pain management is long, but it is gaining momentum.
Keep the conversation in one place—threads here stay linked to the story and in the forums.
Sign in to start a discussion
Start a conversation about this story and keep it linked here.
Other hot threads
E-sports and Gaming Community in Kenya
Active 10 months ago
The Role of Technology in Modern Agriculture (AgriTech)
Active 10 months ago
Popular Recreational Activities Across Counties
Active 10 months ago
Investing in Youth Sports Development Programs
Active 10 months ago